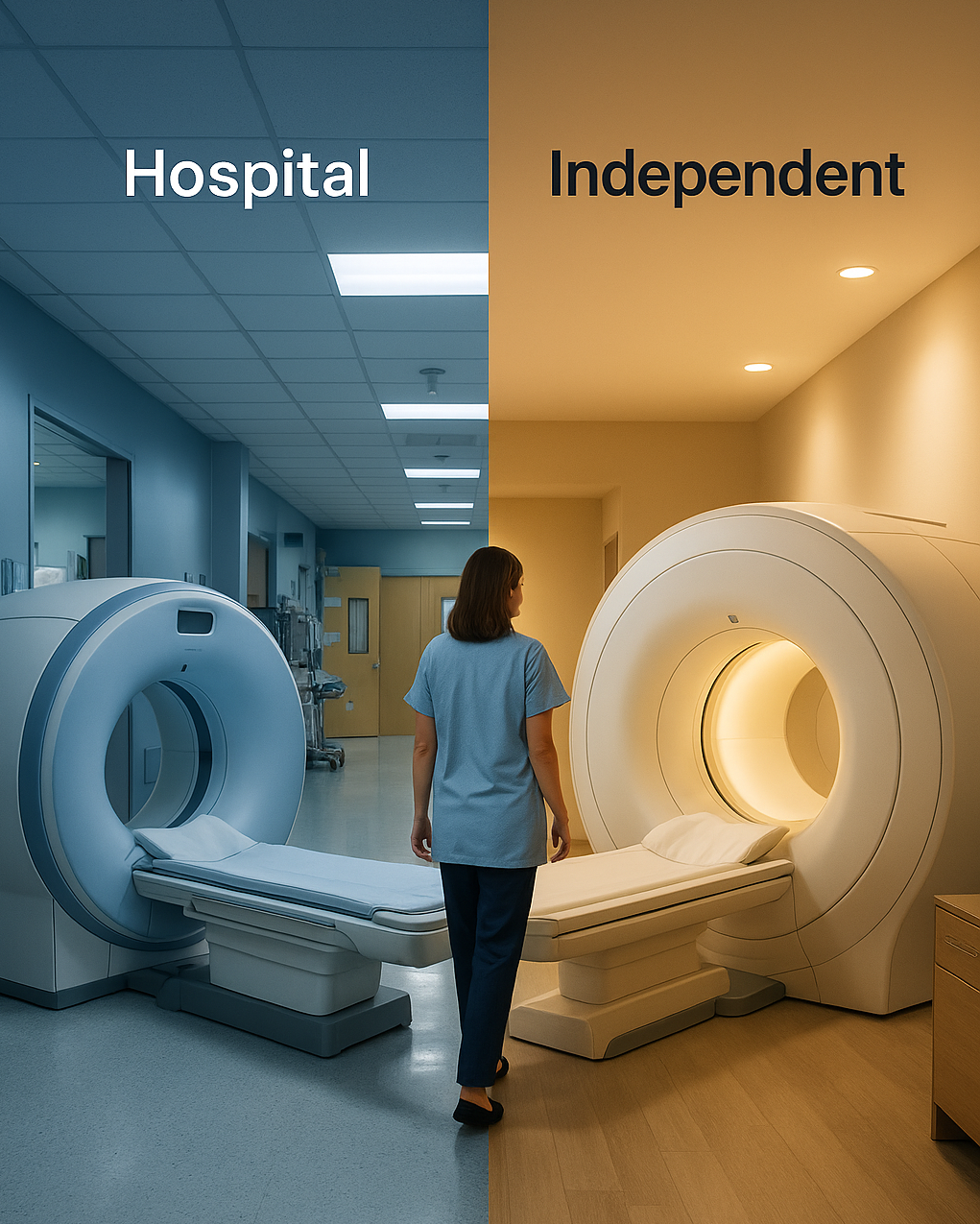
A respected voice in our industry has spent years making a careful, evidence-backed argument: radiology is not a commodity. Diagnostic accuracy varies meaningfully between providers. Steering patients toward high-quality centers improves outcomes and reduces total cost of care.
They’re right. Every word of it.
And they’re solving a problem that assumes the patient is already inside the healthcare system — insured, referred, scheduled, and on their way to a scanner. For tens of millions of Americans, that assumption does not hold.
The question isn’t only which scan the patient gets. It’s whether the patient gets a scan at all.
The quality-first case — and what it leaves out
The case for quality steering is clinically sound. Misinterpreted imaging does lead to missed diagnoses, inappropriate treatment, and downstream costs that dwarf the price of the original scan. Accreditation alone doesn’t guarantee accuracy. Analytics that identify high-performing radiologists can legitimately improve outcomes for patients who reach them.
But this framework starts the clock at a specific moment: the patient has an order in hand and a pathway to a scanner. From there, it asks a useful question — which scanner should they be steered toward?
That’s a good question. It’s not the only question.
Before steering becomes possible, the patient has to be able to afford the scan, find a provider who will see them, and complete a booking without navigating a maze of insurance prior-authorization, hospital billing departments, and opaque pricing. For a large and growing share of Americans, that entire upstream process collapses before quality ever becomes a variable.
What access failure actually looks like
An uninsured roofer in Tampa tears his rotator cuff. His orthopedist orders an MRI. The local hospital quotes $3,400. He doesn’t get the scan. His shoulder heals wrong. Six months later he can’t lift a bundle of shingles.
A small-business owner with a $7,500 family deductible feels a lump. The quoted breast MRI is $2,800 out of pocket in January. She postpones until fall, when she can absorb the bill. The delay is eight months.
A self-employed contractor pays $680 a month for a silver plan with a deductible he’ll never hit in a normal year. His doctor orders a CT for persistent abdominal pain. He calls three imaging centers. None will quote him a price until after he commits. He stops calling.
None of these people received a misread scan. They received no scan at all. And for each of them, the clinical cost of not imaging is larger than any plausible cost of a suboptimally-interpreted image would have been.
Why the access gap persists
The access gap in diagnostic imaging isn’t a mystery. It persists because three structural conditions reinforce each other:
Pricing is opaque by design.
Chargemaster rates, insurance-negotiated rates, cash-pay rates, and out-of-network rates for the same scan at the same facility can differ by an order of magnitude — and none of them are disclosed upfront. A patient who wants to shop faces the same information disadvantage as someone buying a car with the sticker peeled off.
The network is fragmented.
There are roughly 15,000 accredited imaging centers in the United States, operating under thousands of independent ownership groups, each with their own scheduling systems, intake processes, and payment portals. A patient has no practical way to compare them on price, availability, or quality.
Booking is mediated by payors, not patients.
The dominant pathway to imaging assumes an insurance card, a referral, a prior authorization, and a scheduler on the provider’s side who processes all of it. For the uninsured, the underinsured, and the high-deductible, that machinery delivers friction without delivering coverage.
Fixing any one of these in isolation helps at the margin. Solving access means fixing all three at once — transparent pricing, curated national network, direct-to-patient booking — and integrating them into a single experience the patient can actually use.
We’ve solved a version of this before
In 1994, my wife Donna and I founded AnciCare, one of the first nationwide cash-pay imaging networks in the United States. The problem we were solving then is a cousin of the one we’re solving now: injured workers with valid orders and nowhere affordable to get them filled.
Workers’-compensation law allowed employers to direct the care. Independent imaging centers had capacity they couldn’t fill. We connected the two with volume guarantees in exchange for rates below the fee schedule. Over the following years AnciCare grew to more than 1,200 contracted imaging centers and served 168,000 patients, generating roughly $246 million in documented savings before the company was acquired by a public payor.
The playbook worked because it addressed access as an operational problem rather than a clinical one. Quality still mattered — we required ACR accreditation and board-certified interpretation from day one — but the thing that actually moved outcomes was removing the friction that kept patients from getting imaged in the first place.
USRad is the same thesis at a larger scale, aimed at a larger population. Workers’-comp patients numbered in the millions. The population that now pays cash for imaging — uninsured, underinsured, high-deductible, and self-employed Americans — numbers around ninety million. The problem is bigger. The playbook is the same.
What solving access actually requires
Access isn’t a marketing position. It’s an infrastructure problem, and it has three components that have to be built together:
Transparent, all-inclusive pricing. Not estimates. Not ranges. Not “starting at.” A single number that covers the scan, the interpretation, and anything the patient will be billed for, shown before the patient commits. Pricing becomes a decision-making input instead of a post-visit surprise.
A curated, accredited national network. Enough geographic coverage that a patient in any meaningful market can find a center within a reasonable drive. Credentialing standards that meet or exceed what a major payor would require. Pre-negotiated rates so patients don’t have to negotiate one at a time.
Direct patient booking. Scheduling that doesn’t require a referral, a prior authorization, or an insurance card. Intake handled by the platform, not by fifteen different front desks. Payment that happens once, at a known price, with no balance bill arriving weeks later.
Each of these is a necessary condition. None of them is sufficient on its own. A price without a network produces a quote to nowhere. A network without pricing produces a directory of unreachable options. A booking engine without either is a calendar for a store with no inventory.
The next decade of diagnostic imaging
The industry conversation about diagnostic quality is going to continue, and it should. Better measurement, better analytics, and better steering are all real improvements to the experience of patients who are already inside the system.
But the largest gains available in the next decade will not come from making a well-served patient’s scan 8 percent more accurate. They will come from making a scan available to the patient who, under the current model, would have gotten no scan at all. Access is the next frontier — what we call Accessible Imaging — and the organizations that treat it as infrastructure rather than marketing will define what imaging looks like for the people the existing system still fails.
Quality matters. Access is what makes quality matter.
See what accessible imaging looks like
Transparent pricing. A nationwide network of accredited centers. Booking that doesn’t require an insurance card. The access layer, built.
Call us: 1-866-USRad-24 • Mon-Fri 9am-5pm EST